 In 2001, a tragic medication error occurred in a London hospital: a 19-year-old leukemia patient was mistakenly injected with vincristine into his spine (intrathecal administration) instead of through an intravenous line. The drug, intended for IV use, is highly neurotoxic when administered intrathecally. The result was irreversible brain damage and death.
In 2001, a tragic medication error occurred in a London hospital: a 19-year-old leukemia patient was mistakenly injected with vincristine into his spine (intrathecal administration) instead of through an intravenous line. The drug, intended for IV use, is highly neurotoxic when administered intrathecally. The result was irreversible brain damage and death.
This fatal medication error wasn’t caused by incompetence. The clinicians involved were trained, competent, and careful. The true cause lay in poor system design:
- Identical-looking syringes for different routes of administration
- Similar labeling
- Lack of physical and procedural safeguards
This tragedy—one of several similar incidents globally—highlighted a core truth of healthcare delivery:
Even skilled professionals will make errors when systems are not designed with human limitations in mind.
This is the domain of Human Factors Engineering (HFE) a critical discipline now recognized by regulatory authorities worldwide as essential for safe healthcare innovation.
What Is Human Factors Engineering in Healthcare?
Human Factors Engineering (HFE), also known as usability engineering, is the science of designing tools, systems, and environments that optimize human performance and minimize error.
In medical device design, pharmaceutical labeling, and clinical processes, HFE ensures that:
- Devices are intuitive and safe to use
- Errors are hard to make, and easy to catch
- Interfaces and workflows align with real-world user behavior
Key Applications in Healthcare:
- Medical device user interfaces (infusion pumps, ventilators, surgical robots)
- Medication labeling and packaging
- Software as a Medical Device (SaMD)
- Clinical decision support tools
- Drug delivery systems (e.g., auto-injectors, inhalers)
Why Errors Happen: A Systems Problem, Not a Human Problem
The vincristine case is a prime example of latent design flaws leading to catastrophic consequences. It taught the healthcare community that:
- Human error is predictable and often preventable
- Well-intentioned staff can make mistakes under stress, time pressure, or unclear system design
- Blaming individuals doesn’t solve the root problem—designing better systems does
Global Regulatory Requirements for Human Factors in Medical Devices
Increasingly, regulatory bodies require formal integration of HFE and usability testing into product development:
🇺🇸 FDA (U.S. Food and Drug Administration)
- Guidance: Applying Human Factors and Usability Engineering to Medical Devices (2023)
- Requirement: Human factors validation testing is mandatory for devices where user error could result in harm.
- Key Focus: Simulated-use testing with representative users, documentation of use-related risks, and mitigation strategies.
MHRA (UK Medicines and Healthcare Products Regulatory Agency)
- Guidance: Human Factors and Usability Engineering – Guidance for Medical Devices including Drug-device Combination Products (2021)
- Requirement: Manufacturers must apply HFE in the design of medical devices and combination products intended for the UK market.
- Key Focus: Minimizing use errors, especially in self-administration products (e.g., insulin pens, autoinjectors).
EMA (European Medicines Agency)
- Guidance: EMA follows principles under the Medical Device Regulation (EU) 2017/745 (MDR) and ICH Q9 (Quality Risk Management).
- Requirement: For drug-device combination products, usability and human factors testing must be conducted.
- Key Focus: Risk management and clear evidence of safe, effective use under real-life conditions.
Other Standards and Frameworks
- ISO 14971 – Risk Management for Medical Devices
- IEC 62366-1 – Application of Usability Engineering to Medical Devices
- ISO 9241 – Ergonomics of Human-System Interaction
These standards define how to apply HFE from early design through post-market surveillance.
How to Integrate Human Factors Engineering into Product Development
To comply with regulations and build safer products, organizations should embed HFE throughout their design and development lifecycle:
- User Research
Identify target users, contexts of use, and potential pain points. Interview clinicians, patients, and caregivers.
- Task Analysis
Break down how users interact with the product and where risks lie.
- Prototype and Iterate
Design early models and refine them based on user feedback.
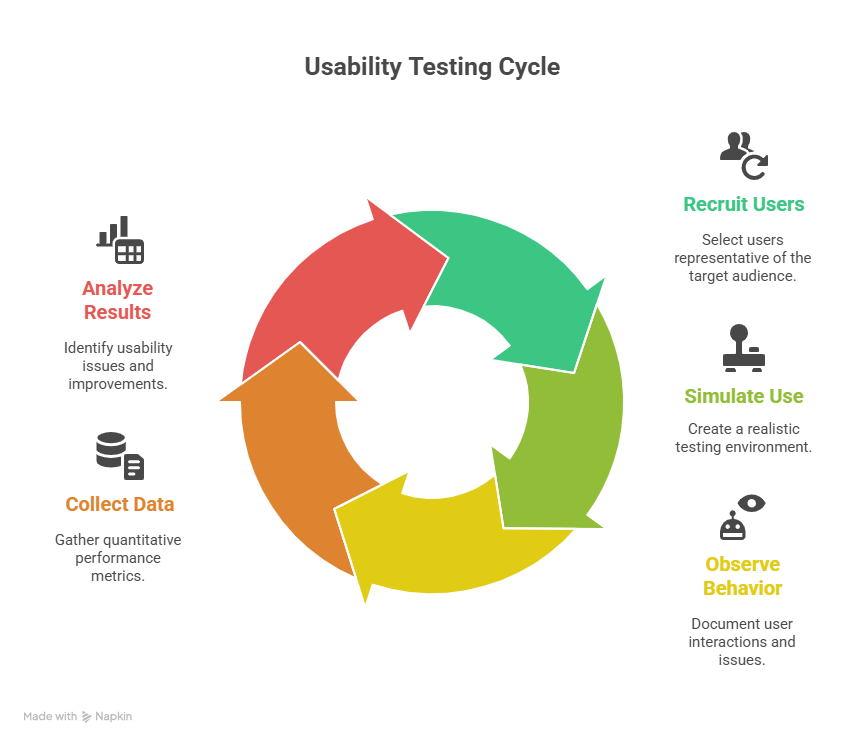
- Usability Testing
Simulate real-world use with representative users. Document any errors or confusion.
- Risk Management
Use HFE findings to inform ISO 14971-based risk mitigation strategies.
- Documentation for Regulators
Prepare detailed usability reports as part of design history files, technical documentation, or 510(k)/CE marking submissions.
Real-World HFE Success Stories
- Smart Infusion Pumps: Embedded drug libraries and soft/hard limits reduce overdose risks.
- Color-coded Packaging: Reduces mix-ups between lookalike/soundalike (LASA) medications.
- SaMD Interfaces: Designed with clear alerts and reduced alarm fatigue for ICU staff.
Each of these improvements stems from understanding how real users think and behave—not how designers assume they will.
The Cost of Ignoring HFE
Medical device recalls, drug administration errors, and clinical inefficiencies often trace back to avoidable usability flaws. More importantly, patients suffer when systems are not designed for safety.
In a competitive market—and a tightly regulated one—companies that invest in Human Factors Engineering early avoid costly redesigns, rejections, or worse: harm to users.
Conclusion: Design for Humans, Not Just for Compliance
The fatal vincristine case was a wake-up call. It taught the world that even life-saving technologies can cause harm when human limitations are ignored.
Human Factors Engineering is not just good practice—it’s a regulatory expectation, a quality imperative, and a moral responsibility.
By designing with people in mind, we build systems that support excellence, prevent harm, and earn trust.